Has your doctor ever told you: “you will need a CS”? Did she give you a reason? I hope she did, because a good number of the 20% of caesarean sections performed globally are likely unnecessary. But more importantly, in Nigeria, we are doing too few caesarean sections (see the first part of this post)—probably because we don’t know when this operation is required.
Whatever the case—too many surgeries or too few—we need to know when a caesarean section is required. Along with information on the safety of the operation, that is exactly what this post will be describing.
A caesarean section—also called a CS or C-section—is a surgical operation used to deliver a baby through an incision in the abdomen and womb.

Reasons for a CS
Broadly speaking, your doctor will recommend a CS either:
- when she anticipates that vaginal delivery would be dangerous for you or your baby,
- or when the baby needs to be delivered as soon as possible and waiting for natural labour is inappropriate.
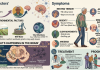
Here are some concrete examples:
Previous C-section: If you have had a previous CS, going through usual labour may cause the scar on your womb to burst open.
Placental abnormality: Sometimes, the placenta can block the mouth of the womb. At other times, the placenta may be too deeply embedded into the womb tissue. These situations can lead to serious bleeding if vaginal birth is attempted.
Multiple-order pregnancy: Triplets and higher-order pregnancies are preferably delivered by CS. Even in a twin pregnancy, if the first twin is positioned abnormally, a CS becomes necessary.
Obstructed or failed labour: If, during labour, you cannot progress—either because there is an obstruction or because you become too exhausted to push—a C-section may become necessary to save both you and the baby.
Big fetus: Also called macrosomia. If, from ultrasound scans and other clues, the baby is estimated to be very big, it may not be safe to attempt vaginal delivery.
Fetal distress: The doctor may detect signs that the fetus is in distress, likely due to reduced oxygen supply. These include an abnormal fetal heart rate or reduced fetal movements. This requires immediate action—which very often translates to a CS.
Breech position: When the fetus at the time of delivery has its buttocks or legs coming out first instead of the head, that is a breech position. While a simple breech delivery can often be handled by a skilled birth attendant, the presence of other complicating factors (like a big fetus or previous CS) may make vaginal delivery unsafe.
Severe preeclampsia and eclampsia: These are disorders in which a pregnant woman’s blood pressure becomes dangerously high, with associated injury to important organs like the kidneys, brain, and liver. The only “cure” is to deliver the placenta as soon as possible, or it may rapidly kill the woman or the baby.
Poor maternal health: Certain conditions, like heart failure, may make it dangerous for the mother to “push” in labour. Others, like HIV or florid genital herpes infection, can be transmitted to the baby during vaginal delivery, making a CS preferable. Other conditions can obstruct the birth canal, such as uterine fibroids, polio, maternal stunting, spine disease, and pelvic tumors.
Is the CS Safe?
The caesarean section is one of the oldest and most refined surgical operations today, and it is considered very safe. It is very possible your surgeon has performed this surgery hundreds to thousands of times before. Moreso, in skilled hands, it can be a brief procedure, lasting about 30 minutes or less.
But for all this, there are still risks.
It is a major abdominal surgery, and you will need up to 6 weeks to recover fully afterwards.
Globally, the risk of serious complications from a CS is low—occurring in about 3–5% of cases in well-equipped settings, though this can be higher in resource-limited environments.
There is a risk of infection of the operation site, wound breakdown, bleeding, and injury to nearby internal organs like the bladder, bowel, and ureters.
Anaesthesia can pose some risk too. Spinal anaesthesia can cause blood pressure to drop critically low. More frequently, however, it causes shivering and headache.
Then there are long-term risks—the chief being that you may require another CS. Also, the risk of abnormal placenta placement in your next pregnancy increases with each CS.
The risk is real, though small. So an unnecessary CS is a no-no. But when your life—and that of your unborn child—is hanging in the balance and a CS is required, I think the risk is justified. Don’t you?